Patient Safety | Surgical Positioning | Operating Theatre Guide
Surgery begins before the first incision. Those quiet minutes while anaesthesia takes hold when the OT nurse carefully adjusts the patient’s position set the conditions for everything that follows. Get positioning right, and the patient wakes up with no positional complications. Get it wrong, and they may spend months recovering from a nerve injury that had nothing to do with what was actually being operated on.
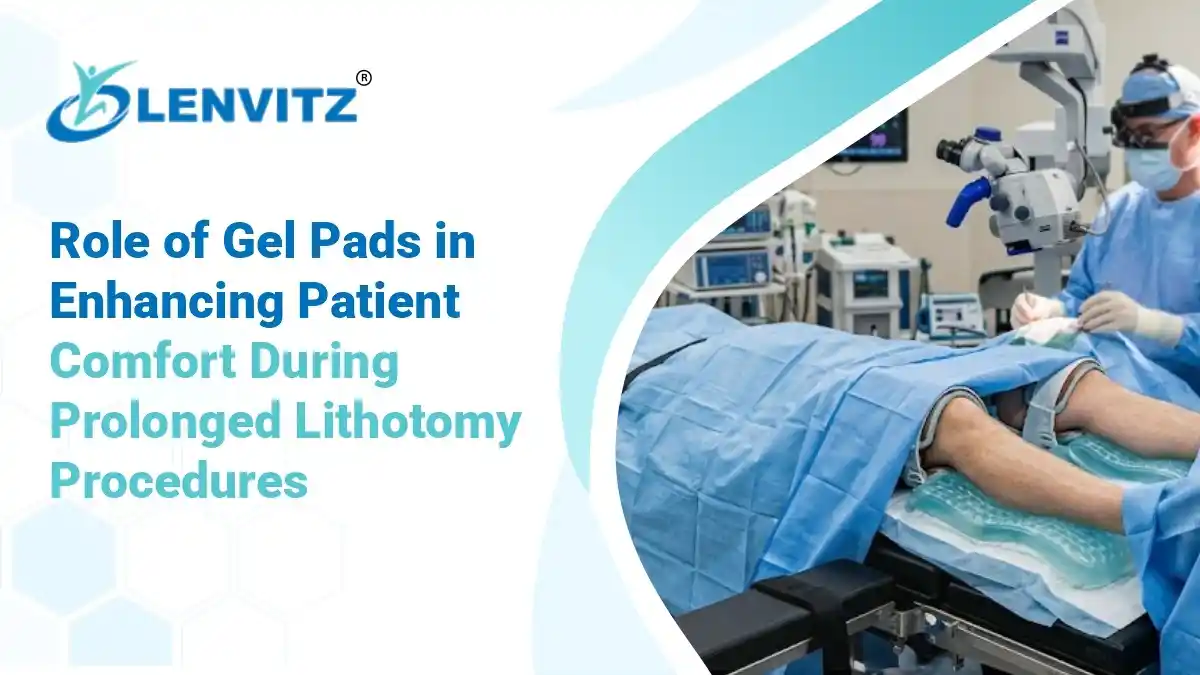
In Indian hospitals from high-volume corporate OTs in Mumbai and Pune to multi-specialty centres in Tier-2 cities the lithotomy position is the standard configuration for gynaecological, urological, and colorectal surgeries including hysterectomy, cystoscopy, prostatectomy, and rectal resection. The patient lies flat on their back with both legs elevated, knees flexed, and lower limbs supported in stirrups. It is a mechanically demanding setup. Hold it for two hours, and the risk profile begins to climb. Hold it for four, and you are in genuinely dangerous territory – with documented cases of foot drop, compartment syndrome, and pressure ulcers all traceable to positioning, not to surgical technique.
The solution is threefold: Lithotomy position gel pads, heel pads, and head ring gel pads each protecting a different anatomical zone, each doing something foam simply cannot sustain over a long case.
What Is the Lithotomy Position?
The lithotomy position is a surgical setup where the patient lies flat on their back, both legs are lifted and placed in stirrups or leg holders, and the hips and knees are bent at specific angles. It is used in surgeries related to the uterus, bladder, prostate, kidney, and lower bowel.
In Indian hospitals, this is one of the most commonly used surgical positions from large city OTs to growing Tier-2 facilities. Gynaecological, urological, and colorectal surgery volumes are rising every year, making correct perioperative positioning and intraoperative patient safety more important than ever.
Why Is Prolonged Lithotomy Position Risky?
The human body is not designed to stay still in one position for hours. When it does especially under anaesthesia, where the patient cannot feel pain or self-adjust serious damage can quietly happen.
A retrospective review of 198,461 surgeries at the Mayo Clinic found motor neuropathy lasting more than three months in approximately 1 in 3,600 cases. The common peroneal nerve which wraps around the lateral fibular head just below the knee was involved in 78–80% of those injuries. A separate prospective study of 991 patients found a 1.5% incidence of lower-extremity neuropathy. Risk factors across both studies: surgery exceeding two to three hours, thin body habitus, and recent tobacco use all profiles highly prevalent in Indian surgical populations.
| Stat | Figure | Clinical Meaning |
|---|---|---|
| Perioperative nerve injury incidence | 0.028–1.5% | Risk is duration-dependent; present in every lithotomy case |
| Lower-limb neuropathies involving common peroneal nerve | 78–80% | Fibular head padding is the single most important protective measure |
| Surgery duration as primary risk threshold | >2–3 hours | The 120-minute mark is when risk escalates measurably |
The 5 Main Risks of Prolonged Lithotomy Position
1. Nerve Damage – The Most Common Risk
The nerve most at risk is the common peroneal nerve it sits just below the knee on the outer side of the leg. If the leg rests against a hard stirrup without padding, this nerve gets compressed. The result? Foot drop the patient wakes up unable to lift their foot properly. Studies show this nerve is involved in nearly 80% of all lithotomy-related nerve injuries.
2. Compartment Syndrome
A rare but dangerous complication. When the legs are elevated for too long, pressure builds inside the muscle compartments of the calf. When the surgery ends and legs come down, blood rushes back causing severe swelling, pain, and in extreme cases, permanent muscle damage requiring emergency fasciotomy. Surgeries beyond 3 hours carry the highest risk.
3. Pressure Ulcers (Bed Sores)
Sustained pressure on bony areas like the heels, tailbone (sacrum), and the back of the skull (occiput) cuts off blood supply to the skin. Over 2–3 hours, this causes tissue breakdown. Indian patients with diabetes or poor blood circulation are at significantly higher risk due to compromised microvascular blood flow.
4. Sciatic and Obturator Nerve Injury
When the hips are bent too far or rotated incorrectly, the sciatic nerve gets stretched. This can cause pain, weakness, or numbness in the leg after surgery.
5. Back, Hip, and Knee Pain
Even without nerve injury, lying with bent hips and knees for hours causes significant muscle and joint strain. Patients often report lower back and knee pain after long lithotomy surgeries a common but underreported complication in Indian surgical recovery wards.
Duration Rule: Clinical guidelines recommend temporarily lowering the legs from lithotomy every two hours for procedures exceeding four hours. Gel pads must be re-checked for correct placement after each repositioning event.
What Are Gel Pads and How Do They Help?
Medical-grade gel pads are soft, cushioned medical devices placed under and around the patient’s body during surgery. They are made from medical-grade viscoelastic silicone a material that moulds to the shape of the body without flattening or hardening over time. It deforms slowly under load and returns to its original shape when the load is removed, distributing body weight across a wider surface area.
Gel Pads vs Foam Pads — What Is the Difference?
| Feature | Gel Pads | Foam Pads |
|---|---|---|
| Pressure distribution | Excellent spreads weight evenly | Good initially, degrades under sustained load |
| Long procedures (>90 min) | Maintains cushioning throughout | “Bottoms out” loses all protection |
| Nerve protection | High moulds precisely to body contours | Moderate |
| Heat and moisture control | Yes reduces skin temperature and humidity | No |
| Shear force reduction | High gel surface moves with the body | Low |
| Best for | All surgeries, especially long ones | Short procedures under 60 minutes only |
Simple rule: For any surgery lasting more than 90 minutes, foam pads are not enough. Gel pads are essential.
Three additional properties that matter specifically in Indian OT environments:
- Microclimate control: Silicone gel dissipates heat at the skin–pad interface. In India’s warm OT environments, heat build-up at a pressure point accelerates tissue breakdown quality gel pads manage both moisture and temperature simultaneously
- Shear force reduction: Shear occurs when skin moves in a different direction from underlying tissue during table tilt or leg repositioning. Gel surfaces deform with the movement in a way rigid foam cannot
- Non-slip stability: A textured anti-slip backing keeps the pad correctly positioned as the surgical table is adjusted, maintaining both patient protection and surgical access
The 3 Key Gel Pads Used in Lithotomy Surgery
1. Lithotomy Position Gel Pads (Leg and Calf Support)
Lithotomy position gel pads are placed between the patient’s leg and the stirrup holder. Their primary protection targets are the calf, the popliteal fossa (the hollow behind the knee through which popliteal vessels and the tibial nerve run), and the lateral fibular head where the common peroneal nerve is most exposed.
What they prevent:
- Peroneal nerve compression → prevents foot drop
- Calf compression → reduces compartment syndrome risk
- Blood vessel compression → protects lower limb circulation throughout the procedure
When to use: Any lithotomy surgery expected to last more than 60 minutes.
Important Procurement Note for Indian Hospitals: The pad geometry must match your stirrup type. Boot-type holders, bar stirrups, Allen stirrups, Yellofin, and candy-cane stirrups all require different pad shapes.
Choosing the right lithotomy position gel pads for your specific setup is critical using a mismatched pad gives false protection and is one of the most common costly mistakes in Indian OT procurement.
2. Heel Pad
The heel pad is perhaps the most underutilised yet critical pad in Indian OT practice. The heel bone (calcaneus) has very little soft tissue covering it. Even moderate sustained pressure over 1–2 hours is enough to cause ischaemic tissue damage.
This is especially critical in India’s surgical population, where diabetes and peripheral vascular disease are highly prevalent. Both conditions compromise microvascular blood flow, making the heel significantly more vulnerable to pressure injury at lower thresholds than in healthy patients.
What a heel pad does:
- Lifts the heel off the surface so there is zero direct contact pressure on the calcaneal bone
- Prevents heel pressure ulcers the most common lower-limb pressure injury in lithotomy
- Controls ankle position to reduce compartment syndrome risk excessive ankle dorsiflexion is an independent risk factor
- Reduces skin friction and shear when the leg is adjusted during surgery
When to use: Every lithotomy surgery lasting more than 30 minutes.
Procurement Tip: There is a meaningful difference between a heel pad designed for supine positioning and one designed for lithotomy-specific boot holders. A flat supine heel pad placed inside a lithotomy boot provides inadequate protection. Always specify the stirrup or leg holder model in your purchase order — not just “heel pad.”
Clinical tip for OT nurses: Always place heel pads before lifting the legs into stirrups not after. Adjusting after elevation can cause skin shear injury.
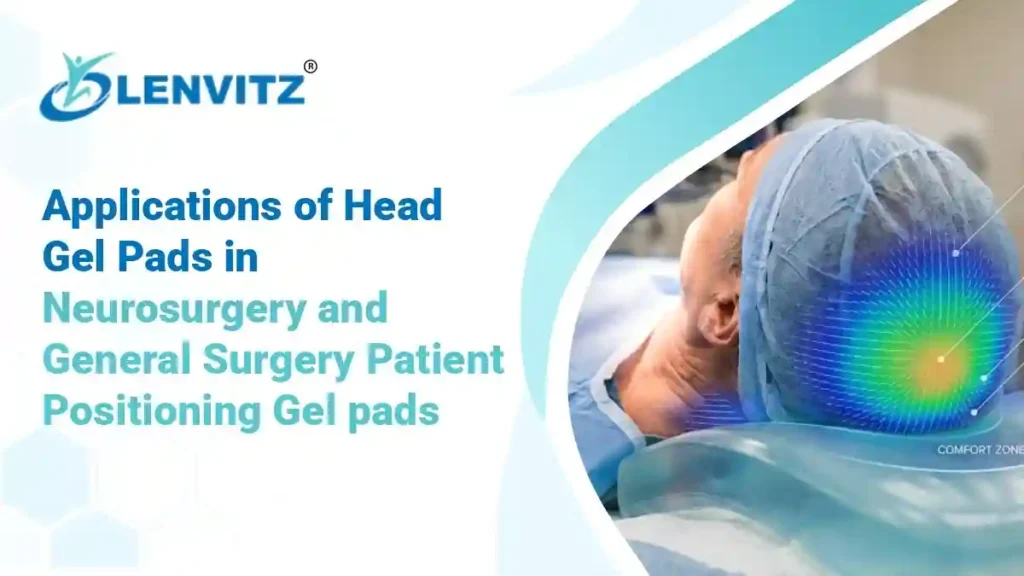
3. Head Ring / Head Gel Pad
The head ring gel pad also available as a head base gel pad is the most overlooked gel pad in Indian OT practice, and that needs to change.
Almost all articles about lithotomy positioning focus only on the legs. But while the surgery happens below, the patient’s head is resting on the hard OT table for the entire duration of the procedure. For a 3–4 hour robotic-assisted laparoscopic hysterectomy or complex rectal surgery, that is hours of continuous pressure on the back of the skull with no movement, no adjustment, and no relief.
The ring-shaped design creates a gap beneath the skull the head rests on the rim of the ring, not on the flat table surface. This dramatically reduces peak interface pressure at the back of the head.
What a head ring / head gel pad does:
- Prevents occipital alopecia – pressure-induced hair loss at the back of the scalp (more common than most OT teams realise, especially in cancer and elderly patients)
- Prevents scalp skin breakdown – in elderly, malnourished, or immunocompromised patients — a growing patient segment in Indian hospitals
- Maintains neutral cervical alignment – reduces neck strain and protects the brachial plexus nerve network in the shoulder area
- Protects ear cartilage – from pressure damage during long procedures — a documented but rarely discussed complication
- Supports airway management – correct head positioning assists the anaesthetist throughout prolonged intubated procedures
- Reduces brachial plexus stretch risk – prevents cervical rotation or lateral flexion that can cause shoulder and arm complications postoperatively
When to use: For all supine and lithotomy procedures not just prone surgeries. This is a widespread misconception. Mandatory for any case exceeding 90 minutes.
Size matters: Head rings come in adolescent size (approx. 5.5″ × 1.5″) and adult size (approx. 8″ × 2″). Always confirm the correct size before placement a wrong-sized ring can create inadequate protection or additional pressure points.
Standard of Care: The head ring gel pad should be on every perioperative safety checklist not just for long cases. The cost is negligible relative to managing a scalp pressure injury or brachial plexus complaint.
Complete Gel Pad Reference Table
| Gel Pad | Protects | Main Risk Prevented | Use From |
|---|---|---|---|
| Lithotomy Position Gel Pad | Calf, popliteal fossa, fibular head | Nerve injury, compartment syndrome | >60 min |
| Heel Pad | Heel bone, posterior ankle | Pressure ulcer, ankle dorsiflexion injury | >30 min |
| Head Ring Gel Pad | Occiput, posterior scalp, cervical spine | Scalp injury, hair loss, neck strain | All procedures |
| Head Base Gel Pad | Full posterior skull, scalp | Pressure injury, cervical strain | All procedures |
| Sacral Gel Pad | Sacrum, tailbone | Sacral pressure ulcers, tissue ischaemia | >60 min |
Choosing the Right Gel Pad: Procurement Checklist for Indian Hospitals
Whether you are a purchase manager at a corporate hospital or a matron managing OT supplies at a nursing home, verify these before buying:
- Material specification: Must be medical-grade viscoelastic silicone not just “soft gel.” Look for ISO 10993 biocompatibility certification
- Stirrup compatibility: Confirm the pad fits your specific leg holder type Allen, Yellofin, boot-type, bar stirrup, or candy-cane
- Disinfection safety: Must survive cleaning with IPA (isopropyl alcohol) or Cidex without cover delamination or gel degradation
- Radiolucent: If your OT uses C-arm fluoroscopy or intraoperative imaging, the pad must not create artefacts on X-ray images
- Size range: Confirm the supplier stocks paediatric, standard adult, and bariatric sizes
- NABH/JCI documentation: Ask for product certificates when submitting for accreditation audits
- Reusability: Know whether the pad is single-use or multi-cycle factor this into your total cost calculation
- Independent interface pressure data: Manufacturer claims without supporting pressure measurement data deserve scepticism
OT Nurse’s Pre-Procedure Positioning Checklist
Use this before every lithotomy procedure. It also serves as documentation for NABH audits and medico-legal records:
- Head ring gel pad placed under the occiput before anaesthesia induction correct size confirmed
- Heel pads positioned under both heels before legs are elevated into stirrups geometry matches stirrup type
- Lithotomy position gel pads supporting the full calf fibular head area (peroneal nerve zone) specifically covered
- Sacral gel pad in position for procedures expected to exceed 90 minutes
- All pad placements re-checked at the 60-minute mark note any visible skin changes
- For surgeries over 4 hours lower legs every 2 hours and re-verify all pad placements after repositioning
- Foam pads not used as substitute for any procedure lasting more than 90 minutes
- All pads used, placement time, and repositioning events documented in intraoperative nursing notes
Frequently Asked Questions
The lithotomy position is used in gynaecological, urological, and colorectal surgeries including hysterectomy, cystoscopy, TURP, prostatectomy, and rectal resection. The patient lies on their back with both legs raised and supported in stirrups, giving the surgical team access to the lower abdomen, pelvis, and perineum.
Clinical risk rises measurably after 90 minutes and becomes serious beyond three hours. For surgeries expected to last more than four hours, guidelines recommend temporarily lowering the legs every two hours to relieve compartment pressure. This is in addition to not a substitute for correct gel pad positioning.
Heel pads should be used for any procedure over 30 minutes. The head ring gel pad should be used in all lithotomy and supine surgeries even short ones because the occiput is always under pressure regardless of duration.
No not for surgeries longer than 90 minutes. Foam pads compress under body weight over time and lose their cushioning effect. Gel pads maintain their protective properties throughout even very long procedures. For short cases under 60 minutes, quality foam may be adequate. Beyond 90 minutes, it is not.
A heel pad is shaped specifically to offload the calcaneus (heel bone). Lithotomy position gel pads are larger and designed to support the entire calf and popliteal region inside a stirrup or leg holder. Both serve different anatomical sites and should always be used together not as substitutes for each other.
No this is a widespread misconception. The head ring gel pad and head base gel pad should be used in all supine and lithotomy procedures, not just prone surgeries. For any case exceeding 90 minutes, the head ring is clinically essential.
Occipital alopecia is pressure-induced hair loss at the back of the skull caused by sustained contact pressure during long surgeries. It is more common than most OT teams realise and is entirely preventable with a correctly fitted head ring gel pad or head base gel pad.
Why This Matters for Indian Hospitals Right Now
India’s surgical infrastructure is undergoing rapid transformation. Hospitals across Pune, Mumbai, Hyderabad, Chennai, and Tier-2 cities are scaling their OT capacities and pursuing NABH and JCI accreditations both of which require documented, evidence-based patient positioning protocols.
Positioning injuries are preventable. A foot drop from a compressed peroneal nerve, a heel ulcer in a diabetic patient, or occipital hair loss in a cancer patient none of these should happen in a modern OT. And they do not have to.
The right combination of lithotomy position gel pads, heel pads, head ring gel pads, and head base gel pads correctly selected for the patient’s body habitus, stirrup type, and expected procedure duration addresses all of these risks simultaneously. These products are inexpensive relative to the clinical and legal consequences of a preventable nerve injury or pressure ulcer. For Indian hospitals serious about patient safety, understanding
how patient positioning gel pads enhance surgical outcomes makes it clear this is one of the highest-return investments in OT quality.